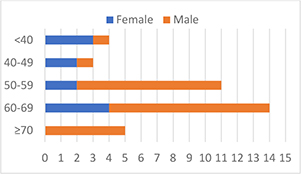
Figure 1. Age distribution by gender
ORIGINAL ARTICLE
Carlan Wendler a, Doug Lindberg b, Greg Sund c
a MD, Director of Emergency Medicine, Kibuye Hope Hospital, Kibuye, Burundi
Professor of Emergency Medicine, Hope Africa University, Bujumbura, Burundi
Adjunct Professor of Emergency Medicine, Keck SOM at USC, Los Angeles, CA, USA
b MD, Director, Center for Advancing Healthcare Missions, Christian Medical and Dental Associations, USA.
c MD, Chief Anæsthetist, Department of Anæsthesia, AIC Kijabe Hospital, Kenya
Introduction: Research as a focus of healthcare missions is an important component of the evolving role of healthcare missionaries and sending organizations in LMICs. There is a lack of data and understanding on what appetite exists to expand and invest in such research initiatives.
Methods: This study surveyed leaders of North American mission sending agencies engaged in healthcare, seeking to ascertain their current and anticipated future involvement in research, education, and healthcare delivery.
Results: Forty-seven leaders responded (of 211 contacted) to our survey of whom 37 completed all survey questions. Eighty-two percent of respondents agreed that they had a responsibility as an organization to study how to improve clinical care and public health. Sixty-four percent of respondents anticipated reduced healthcare delivery in the next 10 years. During that same 10-year, time frame, 61% anticipate an increase in health research mentoring, and 79% expect an increased role of student education. However, this emerging shift towards research and education is not yet reflected with a similar degree of perceived enthusiasm among missionaries in doing research or donors in supporting it.
Discussion: Across the spectrum of middle- and upper-level leadership in a variety of missions sending organizations, there is recognition of an important and increasing role for healthcare research activities in ministry. About half of the agencies represented in our sample are already involved in research and will need to share best practices with others as healthcare missionaries devote more time and attention to research mentorship. Done well, this can provide additional avenues for disciple-making in both home and host cultures as well as improve the care for populations in those remote and rural areas often most served by healthcare missionaries.
Conclusion: Research as mission has, heretofore, been a neglected methodology, but institutional leaders in healthcare missions anticipate an increasingly important ministry role for it.
Key words: global health, research, mission, leadership, mentorship
From the earliest days of healthcare missions, missionary healthcare providers have been engaged in direct patient care and training national providers. In addition to the countless anecdotes in newsletters and blogs, a series of articles on the impact of faith-based healthcare noted that, “the slowly emerging evidence on faith-based health providers suggests that they are not simply a health systems relic of a bygone missionary era, but still have relevance and a part to play (especially in fragile health systems).”1 That role has and continues to change. The Alma Ata Declaration of 1978 encouraged a move from missionary as clinician to missionary as trainer.2 Two generations later, the 2015 Lancet Commission on Global Surgery spotlighted the need for safe and affordable surgical and anesthetic care in addition to primary healthcare.3 As the landscape of global health changes, it is imperative that missionary providers re-evaluate the role they play.4 New tools in telecommunications, remote learning, and international scholarship permit a reimagination of what healthcare missions might look like over the next decades.
As training opportunities continue to grow in many low- and middle-income countries (LMICs), the need for Western missionaries to provide direct patient care will inevitably decrease. As the Church considers the evolving role of healthcare missionaries in the world, a natural progression might be for the cross-cultural worker to aid in developing and deploying systems that allow homegrown providers to collect and disseminate practice-guiding data. While Westerners participate in research in LMICs, this is often performed as “helicopter” research, referring to studies performed by Westerners dropping into a host country to run studies and then publishing findings with little or no recognition of local staff involved.5 Though the challenges to carrying out high-quality data collection and research in low-resource settings are numerous, the Christian belief that every person is an image-bearer requires that it be done in a way that honors all.6 Missionary healthcare providers are in a privileged position to facilitate ethical research done with excellence.
These types of collaborations already exist, as with the Pan African Academy of Christian Surgeons (PAACS),7 a partnership between Loma Linda University and a conglomeration of rural Christian mission hospitals across Africa that has already published numerous academic articles.8-10 To what degree has a trend towards research partnership between missionaries and host communities already begun? How do those in leadership of North American missions anticipate that it will progress? The present study is our attempt to begin to address those questions.
In March 2021, the study authors emailed 211 members of a healthcare missions leadership mailing list soliciting their participation. Most of these individuals are not healthcare workers but are leaders of organizations engaged in healthcare missions. They received an introductory email and a survey link for a 21-item questionnaire administered through the Qualtrics platform (see Appendix 1 for Survey Questions).
The landing page for the survey included a brief description of the study aims and a consent statement which had to be answered prior to continuing to the actual questionnaire. Only respondents who completed all 21 elements were included in the analysis.
For comparisons involving healthcare activity, responses were collated and classified according to a predetermined (5-2-1-0) scoring system according to answers to Items 7-9 (see Appendix). Where appropriate, subgroup comparisons were evaluated for statistical significance by chi-square analysis and student t test.
Forty-seven (47) people responded to the survey invitations of which forty-four (44) opted in and thirty-seven (37) provided complete or near-complete information and were included in the analysis, giving a response rate of 17.5%. Eleven respondents (30%) were female and the majority (51%) were ≥60 years old with four (11%) <40 years old and three (8%) 40-49 years old. Ministry experience was likewise split with the majority (51%) reporting ≥15 years of service in missions leadership. Nine respondents identified themselves with the highest organizational rank of “President / Executive Director / CEO or equivalent,” while five self-identified as “Vice-President / Director of Mission or equivalent.” Two respondents chose “Medical Director/Superintendent or equivalent” and six opted for “Other” with descriptions ranging from “Board Member” to “Program Director.”
The breakdowns of age x gender and rank x age are shown in Charts 1 and 2. Women were represented in all ranks and in every age range <70 years old.

Figure 1. Age distribution by gender
Large missions (>250 fielded units) were the most represented group with sixteen (43%) survey respondents though analysis of their answers to other mission-specific questions indicated that no one large mission was responsible for multiple respondents. The weighting of the missions towards healthcare fell into a tripartite division with fourteen (38%) claiming fewer than 15% of their fielded units being healthcare related, eleven (30%) claiming 15-50% of units being
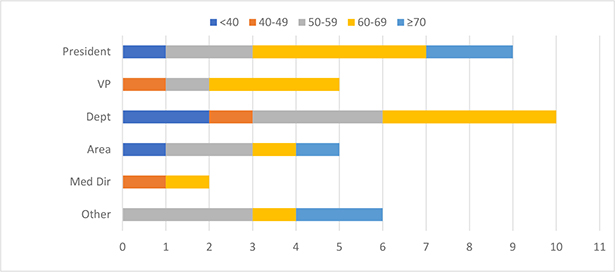
Figure 2. Institutional rank by age
healthcare related, and twelve (32%) claiming the majority of their units were healthcare related.
Table 1 summarizes the proportions of large and non-large missions in each healthcare weighting class.
| Large (>250 fielded units) | Non-large missions | |
| Minimal (<15%) | 5 | 9 |
| Moderate (15-50%) | 6 | 5 |
| Main (>50% healthcare) | 10 | 2 |
When asked to rank their mission’s healthcare activity in three categories, eight (22%) considered healthcare delivery to be their predominant or primary activity, three (8%) considered healthcare education to be so, and none considered healthcare research as such. Using a point system (predominant or primary activity-5, major emphasis-2, minor emphasis-1, minimal or not active-0) to grade overall activity in the three domains, healthcare delivery ranked as most active (70 points), healthcare education second (63 points), and healthcare research as least active (17 points).
Forty-seven percent of respondents reported that someone in their mission had attempted a research project in the prior 24 months while 35% reported that their organization had received some kind of outside assistance for research (including grants, consultation, ethical oversight, etc.) within the same timeframe. If asked by a healthcare missionary for help developing or deploying a research project, 61% of respondents agreed that they could make a contact recommendation immediately, though only 12% agreed that their organizations were ready to pay a consultant to help missionaries conduct research. The median time they thought a healthcare missionary ought to spend on research activities was 8 hours per month (IQR 4,10) though respondents estimated that such only spent a median of 2 hours (IQR 1.25,8) doing so.
Respondents agreed decisively (82% agreed with 18% unsure) that a Christian mission involved in healthcare has a responsibility to study how to improve the clinical care and/or public health of the patients it serves. However, they were less confident (39% agreed with 55% unsure) that the healthcare missionaries in their organizations were eager for more support in doing clinical and public health research with nationals. Even greater uncertainty (30% agreed, 61% unsure) marked their assessment of whether donors to their organizations would be eager to support missionary efforts in clinical and public health research with nationals.
When asked to make a 10-year prediction about the direction of healthcare missions, 18% of respondents thought that healthcare delivery would increase with 64% anticipating it would decrease. Seventy-nine percent of respondents predicted that the role of health student education would increase in the same period, and 61% foresaw a similar increase in the role of health research mentoring. Only two respondents (6%) predicted a decrease in health research mentoring, both of whom predicted an overall decrease in health-related activities in missions. Chart 3 summarizes these results.
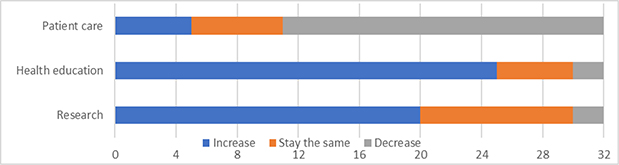
Figure 3. Leaders’ predictions of future direction for healthcare missions (n = 32 responding)
Subgroup analyses of responses to the questions about research attempts and experience, research responsibility and enthusiasm, and the future directions of healthcare missions failed to demonstrate any statistically significant differences on the basis of mission size, healthcare weightedness, or healthcare activity focus though there was a trend towards greater missionary eagerness for research support in those missions that were most heavily weighted towards healthcare missionaries (67% vs 32% in less heavily-weighted missions, p ≈ 0.1).
Demographic comparisons for the makeup of upper and middle leadership in missions organizations are sparse. The email distribution list used for this study was at least 31% female (any indeterminate first names were not counted as female), which tracks with the fraction of female respondents (30%). Some recent studies of physician missionaries11,12 have found women to comprise about half to two-thirds of respondents, though it is these authors’ belief that such is unlikely to accurately estimate the current gender distribution among missions leadership. The age distribution skewed older and more experienced than the authors anticipated with slightly more than half of respondents being aged ≥60 years old and having ≥15 years of missions leadership experience. Given the distribution of institutional ranks represented, one might have expected a somewhat younger sample. If representative, this finding ought to compel a renewed investment in disciple-making within the home office as the next decade will likely see substantial turnover in healthcare missions leadership.
It is no surprise that the largest missions agencies surveyed reported the least focused activity in healthcare. Though one respondent claimed that his mission of >250 fielded units was health specific (100% healthcare or allied workers), the authors were unable to independently verify the identity of that organization.
Likewise, the low estimate of research activity was unsurprising as other methodologies have been ascendant in recent generations. However, the responses regarding missionary time commitments revealed a relatively high priority on research activity. If confirmed, the perceived gap between how much time leaders think healthcare missionaries should spend on research and how much they actually do spend should prompt reflection on what barriers missionaries face in investing in research. An upgrade in missionary and mission research capability is needed, especially when viewed in light of developments in digital communications, data-driven decision-making in missions and healthcare, and the successful implementation of well-trained indigenous healthcare providers in cross-cultural ministry.
No respondent disagreed that a Christian mission involved in healthcare provision has a responsibility to study how to improve the clinical care and/or public health of the patients they serve, and yet, only less than half were aware of any attempts at research from within their missions in the prior two years. If these missions leaders are correct in predicting that healthcare delivery will decrease (64%) and health research mentoring will increase (61%) in the next ten years, then the half of these organizations not doing research will need to pivot towards research mentoring, and the other half will need to share best practices.
High-quality data collection and research in LMICs (where most healthcare missionaries are working) has been neglected for many years. To offer one example, the African Peri-Operative Research Group (APORG), representing over 30 countries and 500 hospitals across the continent, recently drafted their top ten priorities for research in Africa, including establishing evidence-based, practice guidelines, establishment of a minimum, dataset, surgical registry, and improved evaluation of perioperative outcomes associated with emergency surgery.13 All of these priorities present opportunities for collaboration between missionary healthcare providers and their local national partners. Rural district hospitals (where missionaries often work) have been particularly neglected from this global conversation about research and quality improvement.14,15 Healthcare missionaries are in a particularly advantageous position to strengthen (or initiate) research efforts in these settings.
Our study had several limitations. Though above average for this type of survey, our (completed) response rate was 17.5%. As for any opt-in instrument, there is a risk that our respondents represented the most enthusiastic supporters (or opponents) of research in global healthcare missions, which would bias the results. We did not ask any additional demographic information beyond sex, age bracket, and years of experience in missions leadership, and both the invite and the survey were in English, which could leave our sample skewed towards one ethnolinguistic viewpoint, though follow-up correspondence confirmed that at least some non-Western perspectives were represented in the sample. Further, being Christian physician-researchers interested in the role of research in missions, our own bias in favor of collecting data to guide decisions inevitably colored the wording of survey questions, which may reify our perceptions.
Our results suggest that healthcare research is currently neglected amongst healthcare missionaries and their supporting organizations. Given the changing landscape in healthcare, in particular in LMICs, we believe the time has come for these servants to re-evaluate their strategies and priorities to include healthcare-related research and research mentoring in the coming years. This will require a shift in the preparation and training of such missionaries and increased collaboration between Western-based, academic centers and hospitals found in low-resource settings. This needs to be done circumspectly, as history warns of predatory practices, of local partners used for the purpose of data collection and omitted from presenting or publishing the results. However, if done well, research can honor and empower national partners. The results of such collaborations will be increased capacity to achieve local solutions to local problems and a God-honoring unity between nationals and their mission partners. In addition, these efforts may offer missionaries an opportunity to collaborate with Western secular institutions, developing relationships with “unreached” people in the missionaries’ home culture. Best practices for such collaborations are already emerging.16-18
The role of the cross-cultural healthcare missionary is changing as a result of God’s gracious provision for national providers to excel in clinical care and in training their replacements. The waning need in some places for cross-cultural workers to provide direct patient care and technical education opens the possibility for them to devote energy and expertise to research partnerships and mentorships. The disciple-making potential of such relationships is by no means impoverished compared with other healthcare missionary activities and represents a rich vein for cross-cultural collaboration and reciprocal learning.
(After consent obtained)
(Two additional elements pertained to participation in a follow-up interview and processing of a small financial incentive–a donation to the project of the respondent’s choice among 4 pre-selected organizations.)